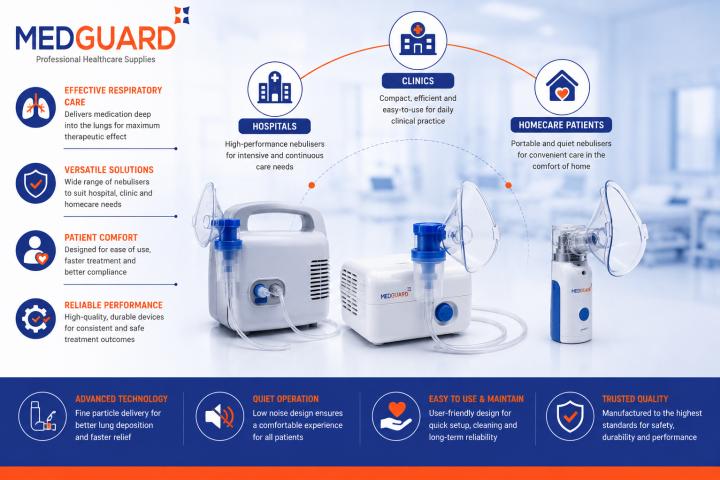
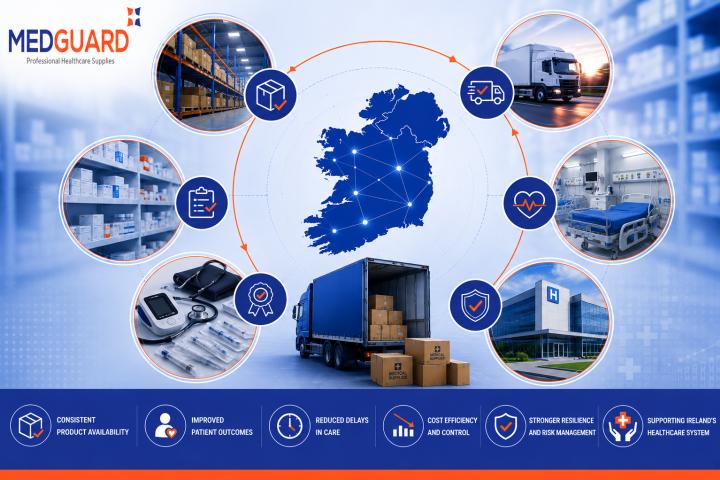
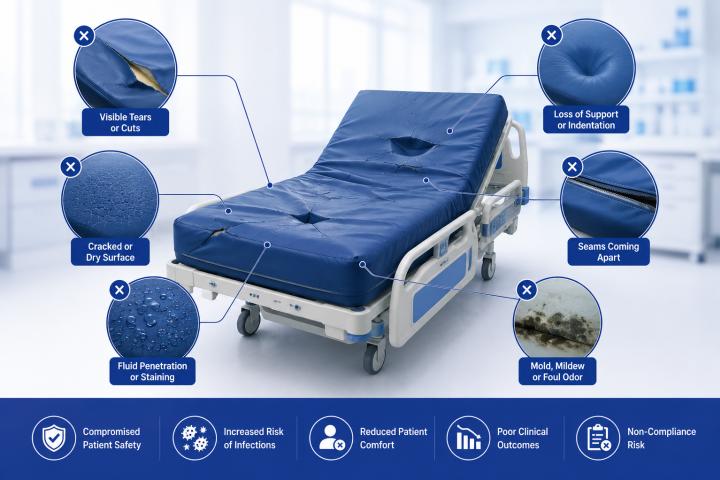
Nebulisers are widely used in hospitals, clinics, nursing homes, and homecare environments to deliver respiratory medication directly into the lungs. They play an important role in treating conditions such as asthma, chronic obstructive pulmonary disease (COPD), cystic fibrosis, and other respiratory illnesses. While nebuliser technology continues to improve, the effectiveness of respiratory therapy depends heavily on proper infection control practices.
Poor hygiene and inadequate equipment maintenance can reduce nebuliser efficiency, increase the risk of respiratory infections, and compromise patient safety. In healthcare settings where respiratory devices are used frequently, strong infection control protocols are essential for maintaining treatment quality and ensuring reliable patient care.
By improving cleaning procedures, staff training, and equipment handling practices, healthcare providers can significantly enhance nebuliser performance while creating a safer treatment environment.
Why Infection Control Matters in Nebuliser Therapy
Nebulisers come into direct contact with the respiratory system, making them highly sensitive medical devices from an infection control perspective. During treatment, moisture and medication residue can remain inside masks, tubing, and medication chambers. If these components are not cleaned properly, bacteria, fungi, and other microorganisms may begin to grow.
Contaminated nebuliser equipment can lead to respiratory infections, especially among vulnerable patients such as:
- Elderly individuals
- Children
- Patients with weakened immune systems
- Individuals with chronic lung diseases
In clinical environments where multiple patients receive respiratory therapy daily, infection risks become even more significant. Proper infection control practices help prevent cross-contamination and maintain consistent treatment safety.
The Connection Between Hygiene and Nebuliser Efficiency
Infection control does more than protect patient safety—it also directly affects nebuliser performance. Dirty or poorly maintained devices may produce inconsistent aerosol particles, reducing the amount of medication reaching the lungs.
Medication residue can clog nebuliser components, restrict airflow, and increase treatment times. Contaminated equipment may also develop unpleasant odors or visible buildup that affects patient confidence and comfort during therapy.
Maintaining clean nebuliser systems helps ensure:
- Accurate medication delivery
- Consistent aerosol generation
- Improved airflow performance
- Reduced treatment interruptions
- Better overall respiratory outcomes
Efficient nebuliser operation depends on both mechanical performance and proper hygiene management.
Establishing Proper Cleaning Procedures
Routine cleaning is one of the most effective ways to improve nebuliser efficiency and reduce contamination risks. Healthcare providers should follow manufacturer recommendations carefully and establish standardized cleaning schedules for all respiratory equipment.
Basic cleaning procedures typically include:
- Washing medication chambers after each use
- Cleaning masks and mouthpieces regularly
- Rinsing components with sterile or clean water
- Allowing parts to air dry completely before storage
In hospitals and clinics, reusable nebuliser accessories should also undergo approved disinfection processes according to infection control protocols.
Moisture left inside equipment can encourage microbial growth, making thorough drying an important part of maintenance. Staff should inspect components regularly for signs of wear, discoloration, or residue buildup that may affect device performance.
Preventing Cross-Contamination in Clinical Settings
Cross-contamination is a major concern in healthcare environments where respiratory devices may be used repeatedly throughout the day. Sharing improperly disinfected nebuliser components between patients can spread harmful microorganisms and increase infection risks.
To improve safety, healthcare facilities should:
- Use patient-specific masks and mouthpieces whenever possible
- Replace disposable accessories appropriately
- Store cleaned equipment in hygienic conditions
- Separate contaminated items from sanitized equipment
Clear labeling systems and standardized workflows can also help staff manage respiratory equipment more effectively and reduce accidental reuse of contaminated components.
Strong infection prevention measures not only protect patients but also help maintain operational efficiency by reducing avoidable treatment complications.
The Importance of Staff Training
Effective infection control depends heavily on staff education and awareness. Nurses, respiratory therapists, caregivers, and healthcare assistants should understand proper nebuliser cleaning, handling, and storage procedures.
Training programs can help healthcare teams:
- Recognize contamination risks
- Follow approved hygiene protocols
- Identify damaged or worn components
- Maintain consistent maintenance routines
- Respond quickly to equipment issues
Routine refresher training ensures that staff remain updated on current infection control standards and respiratory care best practices.
Healthcare facilities that prioritize staff education often experience fewer equipment-related problems and more reliable treatment outcomes.
Supporting Homecare Infection Control
Infection control is equally important for patients using nebulisers at home. Many homecare users are responsible for cleaning and maintaining their own respiratory equipment, making patient education essential.
Healthcare providers should teach homecare patients:
- How to clean nebuliser parts safely
- When to replace accessories
- How to store equipment correctly
- Signs of equipment contamination or malfunction
Simple maintenance instructions can help patients maintain effective respiratory therapy while reducing unnecessary health risks.
Portable and modern mesh nebulisers may also support easier cleaning procedures due to their compact and simplified designs. However, all nebuliser types still require proper maintenance to ensure safe operation.
Long-Term Benefits of Better Infection Control
Improving infection control practices benefits both patients and healthcare providers over the long term. Clean and properly maintained nebulisers:
- Improve treatment consistency
- Reduce infection-related complications
- Extend equipment lifespan
- Lower maintenance costs
- Enhance patient confidence and comfort
Healthcare facilities also benefit from improved operational efficiency, reduced treatment disruptions, and stronger compliance with safety standards.
As respiratory care demands continue to grow, maintaining effective infection control practices will remain essential for delivering high-quality patient care.
Conclusion
Better infection control practices play a critical role in improving nebuliser efficiency and supporting safer respiratory therapy. Proper cleaning, disinfection, equipment maintenance, and staff training help reduce contamination risks while ensuring consistent medication delivery and reliable device performance.
In hospitals, clinics, nursing homes, and homecare settings, infection prevention should be viewed as an essential part of respiratory care rather than simply a maintenance task. By prioritizing hygiene and equipment safety, healthcare providers can improve patient outcomes, strengthen treatment reliability, and create a more effective respiratory care environment.
Original Source : https://www.molecularcloud.org/p/what-makes-nebulizer-use-more-efficient-in-routine-care